As you will have seen, I have been sharing maternity experiences on this blog from women I know. Some good, some bad, some unacceptable. But all anonymous. And it occurred to me that this was somewhat unfair on the birth professionals working to support pregnant women, many of whom I have become friends with on Twitter. So I thought it would be good to be able to share the other side of the story, the thoughts and views of the birth professionals, who have also been afforded the luxury of anonymity. Thus the #MatExp survey was born!

As with everything I do, I JFDI it one evening (thank you for that phrase Florence Wilcock!) and popped it up on Twitter. To my great delight, I have had 150 responses from midwives, student midwives, independent midwives, doulas, obstetricians, anaesthetists, antenatal teachers and other birth professionals. Thank you to everyone who has taken part, your input is much appreciated.
This is the split of respondents:

We also had responses from a neonatal registrar, a perinatal psychiatrist, three midwifery lecturers / educators, a research midwife, two hypnobirthing instructors, an anaesthetist and three antenatal teachers. Many are new to their profession, many have been supporting women for one, two or three decades, and one respondent has been a birth professional for 43 years.
The first thing I wanted to know was “What is the best thing about your job?” The vast majority of respondents talked about the women they work with and being able to support them as being the best part of their role. One student midwife caught the general mood with the comment “Supporting women and being there for them no matter what.” Responses included:
“Witnessing the women I support find their strength and power. Witnessing the love between the couple and the birth of a new little family.” (Doula)
“Being a part of a woman and family’s journey into parenthood.” (Independent Midwife)
“Being part of the transformation of woman to mother” (NHS Midwife)
“Supporting and empowering women, whatever the outcome of their pregnancy” (Obstetrician)
“Making a difference to women. To be present & witness to most beautiful time in life” (Student Midwife)
“Seeing women empowered and birth partners knowing their role and both having calm births” (Hypnobirthing Instructor)
“Privileged to be part of the miracle” (Obstetrician)
Unsurprisingly, the independent midwives found that being able to offer continuity of care and build a relationship with the women they support to be one of the best parts of their job. Many of the obstetricians felt that the best part of their role was “averting danger”, “saving lives”, “helping women to have as healthy a pregnancy and birth as possible”, but also “working with women caring for them at such a life changing moment in their lives” and “being able to reduce anxiety with appropriate explanation”. A fair few of the doulas talked about “witnessing the women I support find their strength and power” and “empowering women”. One explained that the best part of her job is voluntary work “with vulnerable women – asylum seekers, poverty, isolation – who may not otherwise feel worthy of advocacy”.
The word “support” comes up a lot in the responses of NHS midwives, and wonderful comments such as “Making a special time, simply awesome!!!”, “Having the honour and privilege of being a part of a very special time in people’s lives” and “working with the women through an amazing experience”. The student midwives made similar comments, but I particularly liked these two responses:
“The list is endless, but one that currently stands out is being able to turn it around when a woman is panicking in labour and giving them confidence in their own body to give birth! Saying a few words of reassurance and visibly seeing the change is incredible.”
“Supporting women on their journey whatever their circumstances or choices and feeling a sense of fullfillment when you know you’ve made a difference to someone’s pregnancy/birth.”
So from these inspiring comments from people who clearly adore their jobs, we move on to the question “What is the biggest challenge currently facing your profession?” Overwhelmingly the response was NOT ENOUGH MIDWIVES! My recent blog post explores the experience from a woman’s point of view when a unit is short staffed. This really is the biggest challenge as far as these respondents are concerned. Closely followed by fear – “The fear of litigation and professional accountability. The wake of the kirkup report savages midwives and their portrayal is unfair. We may all be tarred with the same brush. Normality is under attack again.” For midwives, morale is also a concern – “we are CONSTANTLY being told what we are doing wrong. Such a culture of fear.”
For obstetricians the challenges are different. Comments included:
“Letting the lawyers decide what information we say and letting them take an additional cut. When the press report a 5.2 million payout the lawyers award themselves a further 6 figure payout.”
“More and more ‘high risk’ women embarking on pregnancies.”
“Too much focus on everything EXCEPT caring for patients!”
“Unnecessary obstetric intervention”
For doulas, they are struggling with a lack of awareness of their role and “dispelling the myth that only the wealthy can afford us”. Lack of awareness from families – “People understanding what support we can provide and the value of it” – and from medical professionals – “Being misunderstood – doulas work alongside NOT in place of HCP”. Some respondents even felt that there is resistance to doulas amongst the medical community.
Where student midwives are concerned, the biggest challenges include:
“Feeling left alone and overwhelmed when its busy because my mentors are rushed off their feet.”
“Bullying… NHS culture”
“Working with midwives who don’t use up to date evidence such a optimal cord clamping”
“Guidelines that seem to have very little evidence base.”
“Bad attitudes, both to those in our care and to each other!”
The over-medicalisation of birth was also mentioned by many respondents.
So what can birth professionals do to meet these challenges? The #MatExp campaign is all about action, and everyone being able to make a difference. Respondents were asked “What do you feel you personally can do to face that challenge?”
Whilst some said “not a lot”, “not sure” and “nothing”, most felt that they had ways to meet the challenges they faced. Answers included the simple “keep on caring”, “keep going” and “raise awareness”. Others said:
“By empowering women to have a voice and question these [hospital procedures]. Also, working together with OBs and MWs to also understand their point of view and what challenges they face. So we can all change this together.” (Doula)
“With 3 colleagues I have set up a social enterprise to provide a caseload midwifery service through NHS commissioning at tariff – the battle is to get it accepted by those who resist changing the status quo” (Independent Midwife)
“Keep going, keep trying to provide compassionate, excellent, evidence-based care, serve the women in my care as best as I can doing my best every shift” (NHS Midwife)
“Not resign myself to that’s how things have to be, think about ways to improve and make suggestions, continue to make every contact with women as positive as possible” (NHS Midwife)
“Show by example how important it is to respect and listen to a woman at all stages of antenatal, labour and postnatal care.” (Doula)
“Ensure that I act within my own values despite others in my environment, find support and positivity from like minded individuals. I love Twitter for that!” (Student Midwife)
“Train our midwives to the highest level to avoid litigation. Test their knowledge to ensure they’ve learned from the training. Keep on asking for more staff and bigger units. Never give up!!” (NHS Midwife)
“Trying to individualise care and support women’s choices Positive birth” (Obstetrician)
“I need to remember I’m a student and should be supernumerary. I need to speak up more to make sure I’m learning each day rather than doing what I know or making beds.” (Student Midwife)
“Continue to practise in the best interests of women rather than defensively and vote against abolition of supervision” (NHS Midwife)
“Try as far as possible to support ‘normal birth’, educate women about the risks of high BMI pregnancies etc.” (Obstetrician)
“Be prepared with an abundance of solid evidence” (Student Midwife)
“Keep my heart strong, separate the bigger picture from the day to day interactions of care, do mindfulness, be compassionate to self, inspire trust in women’s bodies” (Student Midwife)
On a personal note, I particularly like the doula who is determined to be “rigorously evidence-based, and relentlessly compassionate.”
I was keen to see how many of the respondents were aware of the #MatExp Campaign. Many would be of course as the survey started out being publicised to people I knew on Twitter, many of whom I have linked up with due to #MatExp. It gradually worked its way out of that community though, and by the time the survey closed the split was as follows:

The orange line is “I have heard of it but don’t know a lot about it”.
I then outlined the aims of #MatExp as they appear on the NHS Change Day website


The next question was “What do you feel you can do to support these aims?” Many respondents felt that renewed or continued work with their MSLC (Maternity Services Liaison Committee) was the answer. Others simply want to “spread the word” and “let mums know”. Other comments included:
“I encourage women to speak up about things they’re not happy with. Raise it at a higher level if you have to, use the SoM or similar. Empower women so they don’t feel intimidated by professionals telling them what they are and are not ‘allowed’ to do.” (Doula)
“Ensure patient feedback is received acknowledged and acted upon. Continue daily ward visits” (NHS Midwife)
“Support AIMS [Association for Improvements in the Maternity Services]” (Independent Midwife)
“Keep banging the drum for parity of esteem for maternal mental health” (Perinatal Psychiatrist)
“Keep raising awareness on Facebook, hold antenatal classes, tell all the women I come across everything is in their power – try to banish the word ‘allow'” (NHS Midwife)
“Probably the friends and family questionnaires would help and I can make sure these are handed out.” (Student Midwife)
“As a researcher I can help to make maternity service user views more visible and I am also doing a lot of work around ways to increase opportunities for service users to get involved in research/maternity service improvement activities. I am also very interested in the idea of co-creation in research (so working alongside service users and frontline staff to develop, do and use research). Part of the work I am involved with at the moment involves empowering pregnant women and midwives to use research evidence more effectively.” (Research Midwife)
“I’m an increasing Twitter user. Social media seems to be the way forward” (NHS Midwife)
The next question looked at the specific areas that the #MatExp campaign covers, including the area for which I am one of the champions: “Life with a new baby”. The full list is:
Skin-to-skin – see Jenny Clarke’s video
Optimal cord clamping – meet Amanda, optimal cord clamping champion
How does lithotomy feel as a woman in labour – read about obstetrician Florence Wilcock’s NHS Change Day lithotomy challenge
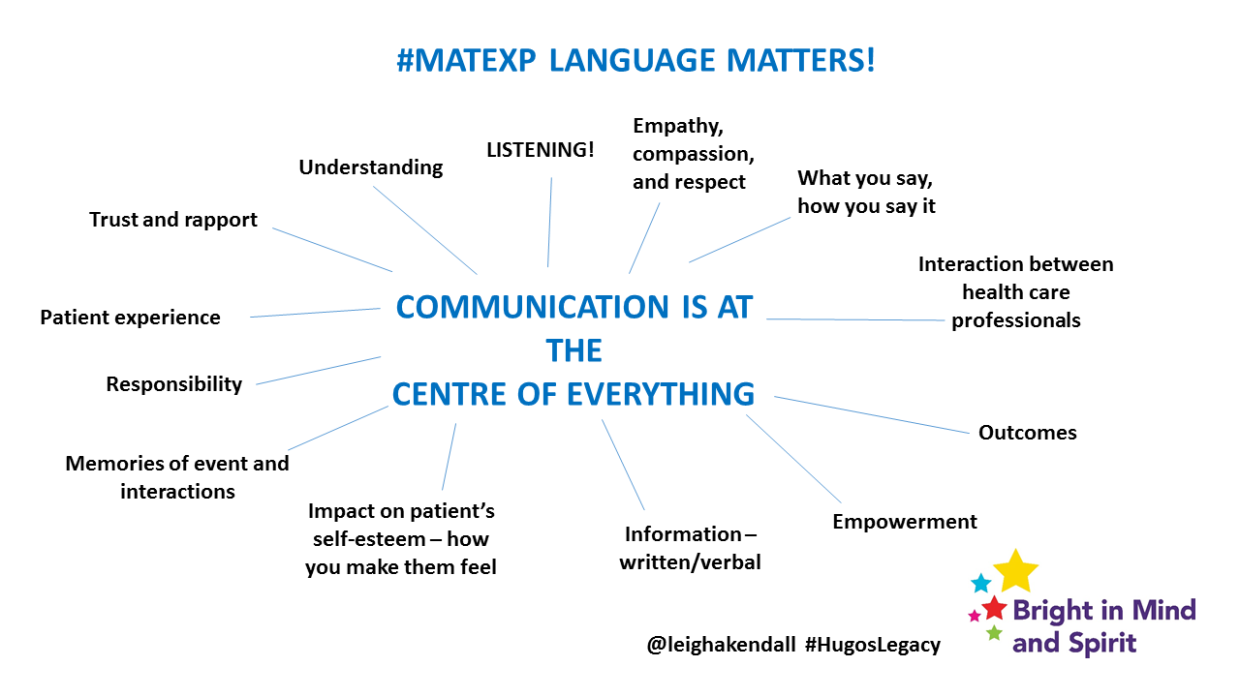
Language used towards pregnant women (e.g. “failed induction”, “poor maternal effort”) – this area is championed for the campaign by Leigh Kendall
Life with a new baby – including perinatal mental health and breastfeeding. Read about Rosey PND&Me and also the blog post that Emma Sasaru and I put together on supporting breastfeeding.
Informed Choice – see this example of risk being explained in a user accessible way
Respondents were asked to rank these areas in order of importance and the results were:

A couple of respondents had (very fair) specific comments on the above question, namely “our unit is already changing skin to skin and delayed cord clamping, hence their low ranking, otherwise I would have placed them higher, my next project is to reduce the use of lithotomy” (Obstetrician) and “it is impossible to rate these in order. In general they each impact on each other, by improving informed choice you are creating a healthier postnatal environment etc. so rankings don’t mean that skin to skin is the least important” (NHS Midwife).
The response to the next question was fairly definite!
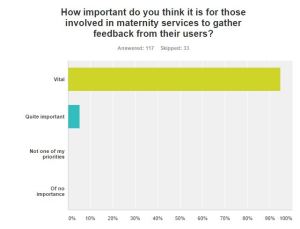
Finally, I asked “If you could change one thing about maternity care in the UK what would it be?” Staffing levels were mentioned again by a lot of respondents, as was caseloading / one to one care. Many of the answers were also indicative of the tensions between different birth professions and professionals:
“For more medical staff to witness natural birth.” (Doula)
“Doctors and midwives respecting each other” (NHS Midwife)
“Obstetricians” (NHS Midwife)
“If we loved and treated our colleagues better, collaborated and supported each other, we’d be a happier, more efficient more compassionate and passionate workforce- and this would filter through to the women we support” (NHS Midwife)
“Reduce obgyn lead care.” (Doula)
“NCT didn’t have such a negative influence on women. No one failed because they didn’t have a vaginal birth. A lot of what is taught is inaccurate and based on personal opinion which is not informed choice.” (NHS Midwife)
“Slow down the relentless overuse of induction…encourage/ optimise midwife led care home birth and birth centres and caseloading model of care.” (Student Midwife)
“Don’t always go and try to enforce your procedures. Listen to women. Use of language for the purpose of influencing a labouring woman into accepting the best thing for hospital such as I witnessed: ” This baby has had enough” is very detrimental, and to say the least, manipulative.” (Doula)
“I would offer a single additional session to antenatal classes/NCT classes etc about the reasons for medical interventions in labour and the risks and benefits. It is unbelievable that in an age of information, when women have spent time with midwives and NCT instructors, we still regularly see birth plans that say “don’t want forceps unless necessary”! It immediately disadvantages obstetricians and puts them on the back foot, as we not only are seen as “the bad guys” for forcing these interventions on women, but often have a matter of minutes to explain the risks and benefits in an urgent situation, which is frankly laughable. Obstetric trainees should be involved in antenatal education; just a single group session on the what, when and why of CTGs, forceps, FBS and Caesarean would I think remove a lot of the fear from women and help those for whom labour does not progress smoothly to feel more empowered and informed.” (Obstetrician)
“More trust in women to make the right choices for themselves. Less bullying and misinformation.” (Independent Midwife)
“Obs and midwifery attitudes to each other.” (Anaesthetist)
I would also like to highlight this heartfelt plea from an NHS Midwife: “I don’t even know where to start… Let’s be compassionate again – let’s treat EVERY woman like our sister. Even the smelly, rude, unpleasant ones. Let’s try.”
Along with a number of #MatExp participants on Twitter, I have been saying that respect and compassion are two vital elements of a positive birth experience, regardless of vaginal birth, c-section, place of birth and so on. This comment from a doula certainly chimes with my personal view on what could change in UK maternity care: “I’d like it to be less of a lottery, some professionals are kind, supportive, informed, happy to discuss options with women. Some are not. On the same wards, in the same hospitals too. I’d like the good experiences that many have to be normal for all. The feedback I get is this comes down to how the woman is treated rather than the final outcome of the birth experience.”

The full results of the survey have been passed to Florence Wilcock, #FabObs of the #MatExp campaign.