One night when I was 23 weeks’ pregnant, I woke up with a pain in my chest.
“Heartburn,” I thought.
It was uncomfortable, I felt constantly full. Normal heartburn medicine did nothing.
I was putting on a lot of weight. Normal for pregnancy, I thought.
I was becoming breathless. Related to the weight gain, I thought.
I was very emotional. Normal pregnancy hormones.
I Googled my symptoms. Preeclampsia was a possibility. “Don’t be ridiculous,” I thought, “I am only 23 weeks’ pregnant.”
This went on for six days. Getting progressively worse.
The heartburn became painful. I was unable to sleep. I got up in the night to drink milk. I don’t like drinking milk. I even resorted to taking paracetamol, having resisted any drugs in my pregnancy until then.
Day seven brought a routine midwife appointment. High blood pressure. Ridiculously high. Surely the machine must be broken, I have low blood pressure. Three pluses of protein in my urine. I had to go straight to hospital for further checks.
I knew the protein was a symptom of preeclampsia, but I was not worried because I was only 24 weeks pregnant. I thought it was a problem only in later pregnancy. I thought I would be bored in hospital. Lots of waiting around. I had forgotten my Kindle.
How wrong I was.
Arriving at Bedford Hospital, more urine given, blood taken.
A consultant comes to see me. I have preeclampsia and something called HELLP syndrome. Everything else is irrelevant because they say I will have to deliver my baby that night. I am seriously ill, and the only cure is to deliver the baby.
It is early, far too early.
I am distraught. So is Martin. We cannot believe it.
An injection is put in to my thigh. It hurts. But it is a steroid, to help my baby’s lungs develop. It is the first of two such injections.
I am taken to a room that doubles as an operating theatre. I have to remove all my clothes and put on a gown. I am advised to remove my rings, because sooner or later my whole body will swell and they would have to be cut off.
A catheter is inserted. I do not understand at that time the concern for my kidneys. I am sure someone must have told me, but I do not remember. It takes me several weeks to figure out the connection.
I must have a cannula so they can give me magnesium sulphate to protect my and my unborn baby’s brain from potential seizures. A doctor tries, then the consultant. Anaesthetists are called. They try, one arm each. So many attempts, but the cannulas do not flush through. I am able to count 20 puncture marks when the bruises appear later that week. Martin leaves the room because he cannot bear to see me in such pain.
Mercifully, they give up and insert a central line. I lie perfectly still, a plastic sheet over my head as they insert a line into my jugular. It is stitched into place. It is difficult to move my head.
They start the magnesium sulphate through the line in my neck. All of a sudden I am on fire. My skin is burning. I throw up.
A radiographer comes to take an x-ray of my chest, to make sure the central line is in the right place, not poking into a lung. A lead apron is placed over my belly to protect the baby. I am asked if I am happy having an x-ray because I am pregnant. “Of course I am not bloody happy about it,” I reply. But what choice do I have? A punctured lung not do me or my baby any good.
I am told I my baby will have to be born that night. There will be no time to induce me, so a Caesarean section it is. An epidural is out of the question because my platelet levels are too low. A general anaesthetic it will have to be. My baby is too small to be cared for in that hospital so will be immediately transferred elsewhere, with me following when stable enough.
Platelets are what enable the blood to clot. An epidural could cause bleeding in my spine and leave me paralysed. I do not want to be paralysed, but nor do I want my baby to be sent away from me, with the chance that I will never meet him.
Two neonatologists come to see me. This hospital is equipped to care for babies from 34 weeks. My baby is far too early. I can see the fear and uncertainty in their eyes. They say there is a 50/50 chance whether our baby will be born alive. If alive, he is likely to suffer a short, painful life because of brain bleeds and bowel problems. They ask us if we would want them to attempt resuscitation. We do not hesitate to say we want our much-wanted baby to be given every chance. We are terrified.
This is Monday night. Martin sleeps on a reclining chair next to me. Except neither of us sleep. We both sob, mourning the baby we have not yet met.
I am given hourly checks on my reflexes. I am not allowed to eat, with the possibility of a general anaesthetic soon. I am allowed only enough water to swallow more medication. I am attached to a blood pressure machine and a sensor on my finger to monitor my heart rate.
Morning arrives. My baby is still in my belly. Relief! I am feeling much better. I am allowed to eat, but my fluid intake is still strictly monitored. My mum arrives, having set off early that morning and driven all the way from Devon.
The doctors are puzzled. My condition has stabilised, and some things have even improved. I am special. The kind of special that no one wants to be. I am still not going anywhere though. I am forbidden from getting out of bed. They are waiting for me to be stable enough to be transported to a bigger, specialist hospital. Wherever has a spare bed.
A student midwife is posted next to my bed all day. I am glad, I have someone to chat to. I do not realise at that time that she is there not for my entertainment, but in case I suddenly have a seizure, or otherwise suddenly deteriorate.
The midwives consult the procedure for the care of women with preeclampsia, it is something they see so rarely. They are kind and different ones pop in to see me to see how I am getting on.
A friend visits. While she was there, she tells me months later, the consultant arrives. He tells me I am seriously ill and that they are very worried about me. “Oh ok!” I apparently cheerfully reply. My friend is terrified. I remember her visiting, but I do not remember this conversation.
I am completely, blissfully, away with the fairies.
That night Martin returns home to sleep. There are more hourly checks. Some people turn on the wrong light switch, turning on the dazzling theatre lights. The infusion machine seems to be programmed to occlude and alarm every time I drop off to sleep. I am exhausted.
Wednesday morning arrives. I am allowed to get out of bed for the first time since Monday evening. I waddle to the shower to sort of get clean – I am told to try to not get my central line wet.
A bed has been found for me at St George’s Hospital, in south London. Liverpool was next on the list. I am happy with south London. In fact, I don’t really care. An ambulance has been called to take me there. Two midwives will accompany me. What an overreaction, I think, I feel much better than I did on Monday. Martin is unable to come in the ambulance, not enough room, so he follows by train.
We speed down the M1, blue lights and sirens blaring. Zoom through central London. The ambulance is uncomfortable, lying on a stretcher.
I arrive at St George’s. Taken to another private room. The midwives and paramedics wish me well and depart. My history is taken by more doctors. They say I will be moving to another room, one with more monitoring capacity, but first they need to move the woman currently in there out: I need it more. The severity of my illness still doesn’t dawn on me.
I am taken in a wheelchair for Doppler scan. It is a busy waiting room. People stare at me in my bottom-baring gown, central line, catheter, and generally looking a mess.
Martin and I are excited at seeing our baby on the screen. We are told our baby is growth-restricted, but I am mesmerised. The sonographer apologises, she would like to explain more but it is a rush, it is the end of the day, and she needs to get the results to the consultants. We are given an appointment for another scan in a week’s time. Hope.
I wait in the corridor for a porter to take me back to the ward. My heartburn is getting worse. I feel so sick. The pain is awful. I just want someone to take the pain away. Back on the ward, I do not know what to do myself. The pain! I stand by the bed. I start to shake uncontrollably. I am given medication, the pain goes away. I feel so much better.
That night I sleep so well. Martin is on a mattress on the floor next to me. I have my hourly checks. The baby’s heartbeat is strong. Everything feels ok. I will wait in this bed for a few weeks, let my baby get bigger and stronger before he has to be born. I will be bored out of my mind, but that will be ok.
I do not have time to be bored.
Thursday morning, a contingent of consultants arrive. They ask me how I feel. I say I feel really good: I have finally had some decent sleep, and the pain has gone. They say I am not ok – my baby will have to be born that morning. For real, this time.
I sob and sob. It is too early, far too early. We were going to have more time. I am given an examination to see if I can deliver naturally, but my cervix is locked shut. A Caesarean it is. Martin holds one hand, a kind doctor another. Both try to reassure me. I ask whether my baby will be born alive. They cannot say. They tell me how ill I am, apparently. I do not remember.
Anaesthetists arrive to explain what will happen. I listen but I do not hear, I am too distressed, and anyway I do not care. A consultant explains the risks of the section: bowel and bladder rupture, the chance of no more babies. I do not care, do whatever you like to me, make sure my baby is ok.
I am wheeled down to theatre. I feel like the worst mother ever: knowing my baby is likely to die so my life can be saved. A strange calm comes over me. I accept that I am unlikely to meet my baby. We will get a dog, and go on a holiday when I am better. Martin and I kiss and cuddle. He is not allowed in theatre with me. I tell him our baby is going to be called Hugo. I liked that name, but we had not been able to agree on a name for our unborn son.
One anaesthetist gives me a fluid to drink to stop my stomach acid rising. I am told to down it in one, like a shot. They are both so kind. But this isn’t going to be a good time. They need to put more needles and lines in me. I am given a sedative so they can do that. That is the last thing I remember.
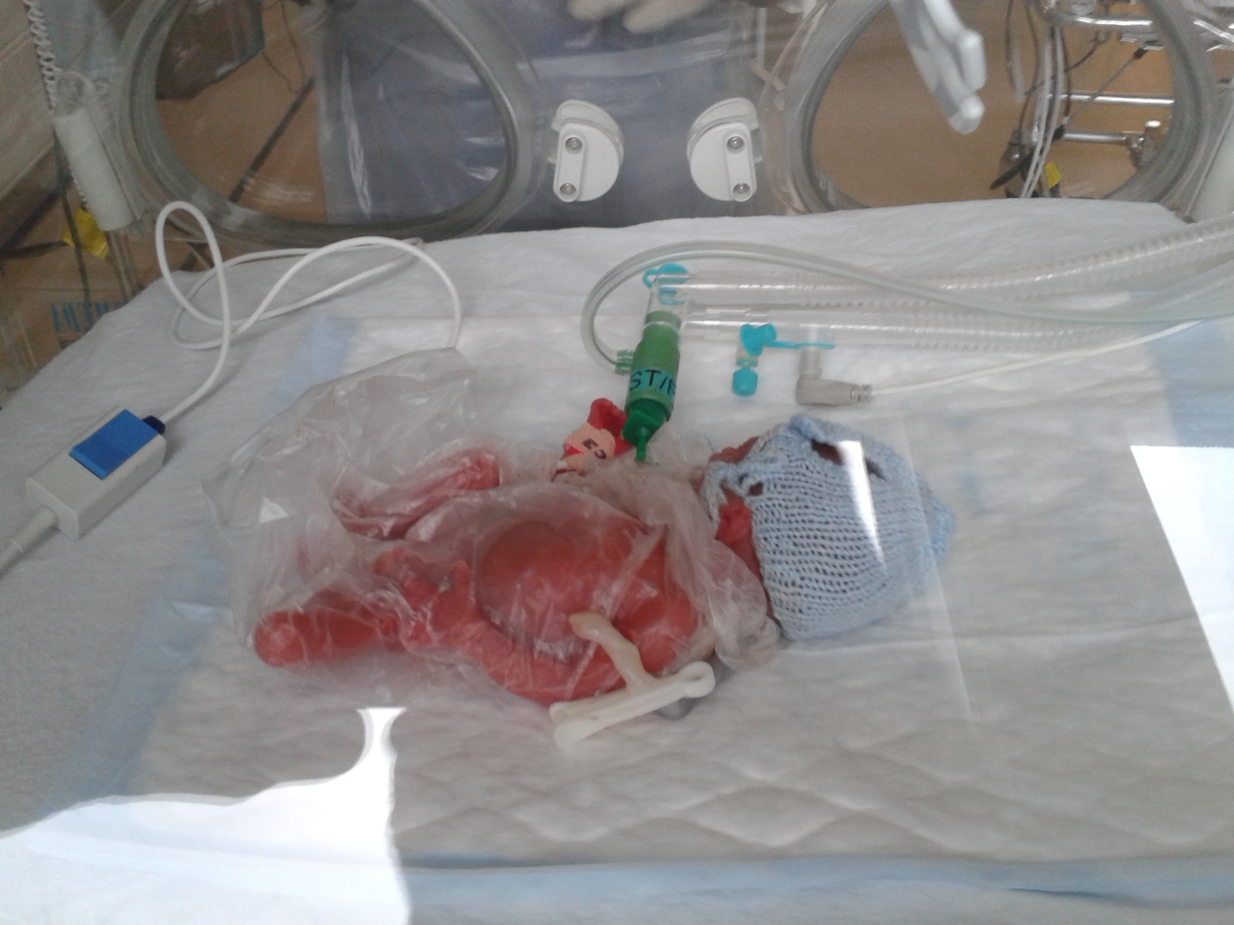
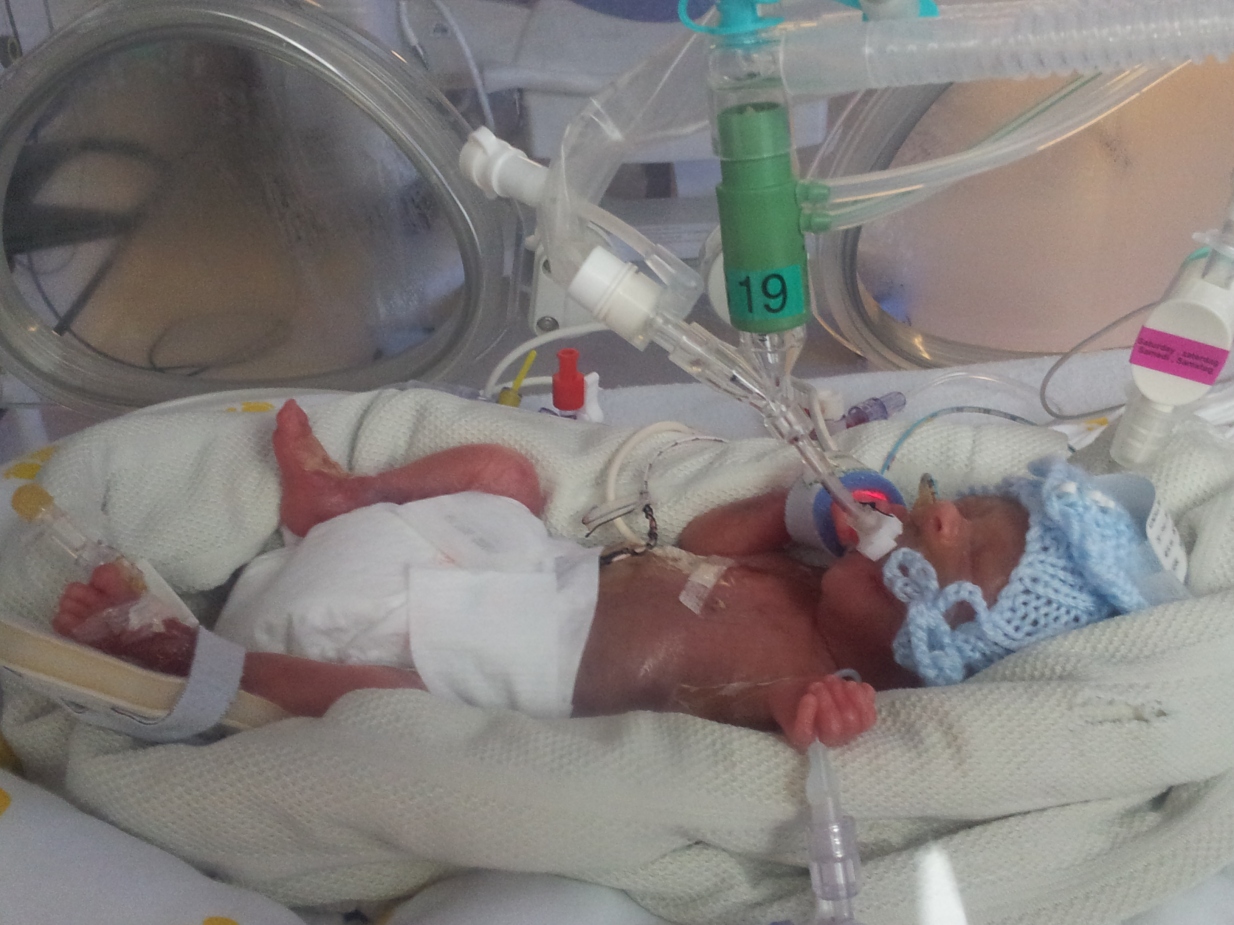
Hugo is born at 11.20am, weighing just 420 grams. He is ventilated and whisked off to the neonatal unit. Martin is there when I wake up. He tells me Hugo is alive. I give the biggest smile. I do not remember this conversation, nor do I remember him holding my hand while I am wheeled all the way to intensive care, the other end of the hospital.
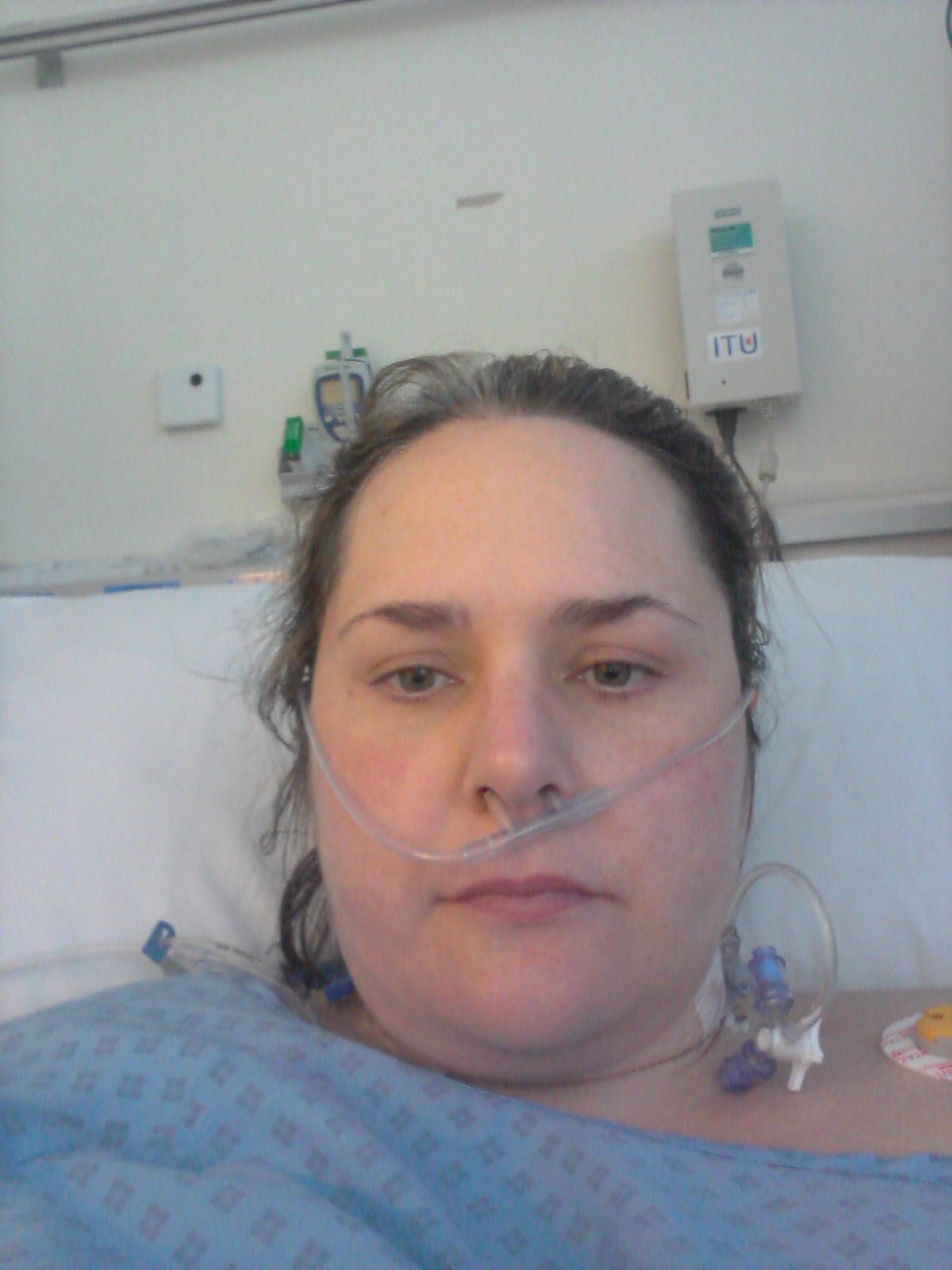
I remember the nurse saying my name, trying to get me to wake up. I have more wires. One in my wrist marked ‘arterial’ to measure my blood pressure. A drain coming out of my tummy. Oxygen prongs up my nose. More magnesium sulphate being pumped in to me.
I just want to know about my baby. I want to see him, to be with him. I am told that day is impossible. I need to rest. There is still danger even after the baby is born. I lost two pints of blood during the section. I am swollen everywhere. I cannot grip anything with my hands. My mum feeds me fruit yogurt, I cannot use a spoon.
A consultant visits to see how I am getting on. Tells me “Sorry we had to do that to you, your organs were about to fail.” “Oh, that’s ok!” I brightly reply. Oh, blissful morphine had taken me even further away with the fairies .
A midwife arrives to express some of my colostrum for Hugo. Precious protection for my little boy. One thing I can do for him.
I feel totally helpless. There are so many beeps and alarms on this ward. I cannot move.
Martin says how amazing Hugo is, a beaming smile. I have photos of him. Precious photos. I want to see him myself. I cannot wait to be with my baby.
Friday morning arrives. I am told I can leave intensive care, and return to maternity high dependency. I will be taken to see Hugo on the way. I cannot wait.
Time ticks away on that Friday. For the previous day and night I had my own dedicated nurse, and now I share her with another patient. They take up most of her time.
I feel alone, helpless, and want to see my baby more than anything else in this world. Why do they not understand?
I ask, so many times. Nurses make calls. A problem with the bed I need. I do not care, I want to see my baby. My baby needs his mummy, I need my baby. No one takes me. No one does anything about it.
By the end of the afternoon I ask the nurse caring for the patient next to me (bizarrely, my nurse’s other patient is at the other end of the ward) if she knows when I will be taken to meet Hugo. I do not remember her exact words, but they were to the effect of “Pipe down, there are other patients much sicker than you on this ward.”
I am so upset. I am in a hospital a long way from home. I do not even know what this hospital looks like. My body has not been my own this week. I need care, compassion, understanding.
Eventually, at around 8.30pm they decide they will take me in a wheelchair to meet Hugo. At last! It is a delicate operation, I am swollen like a Michelin man, I have wires going into me and going out of me. I am not able to move alone, and have not mobilised since the C section. The curtains around my bed are drawn to preserve my modesty.
Suddenly Martin’s head appears in a gap between the curtains. I am not to worry, he says, but I need to come quickly. I can read the look on his face: there is much to worry about. I make him tell me: Hugo’s blood pressure is declining, and nothing they are doing is working. They are worried they are losing him.
I shriek. Shout at the nurses with their faffing. They are trying to be gentle with me, I know, but I am unspeakably furious at them for the time they have taken to take me to see Hugo. I am terrified he will die before I get there.
The nurse wheels me along the corridor. People get out of the effing way! Don’t they know my baby is dying? The wheelchairs are as bad as supermarket trolleys, she wheels me into obstacles. The pain shoots up in to my stomach wound. Martin takes over.
We get to the neonatal unit. Hugo’s nurse and consultant introduce themselves. They had been frantic, but the little monster’s blood pressure corrected itself the moment I arrived.
Little Hugo Boss knew exactly how to get what he wanted. His mummy.
I shrieked again when I saw him. So small, so red.
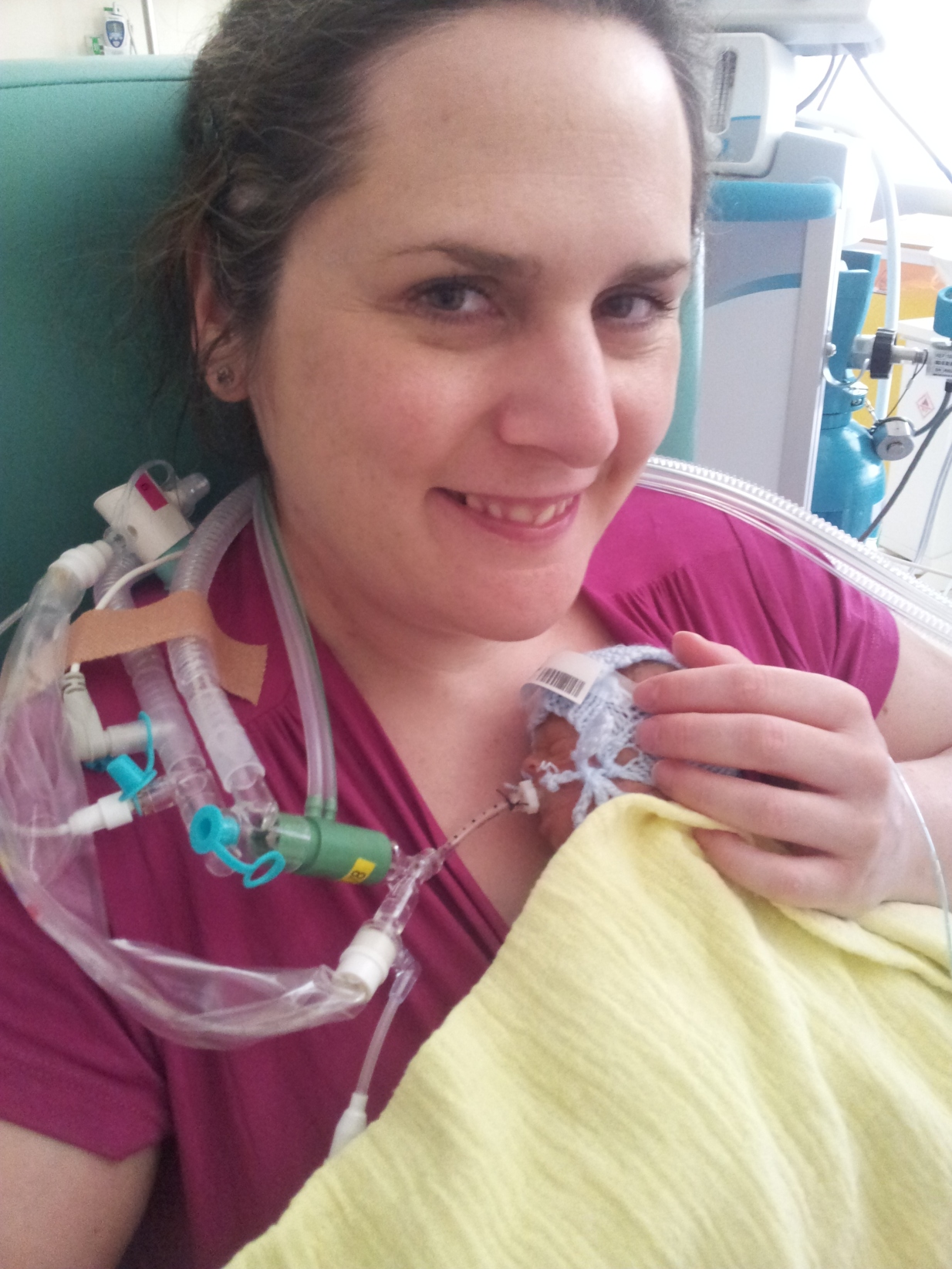
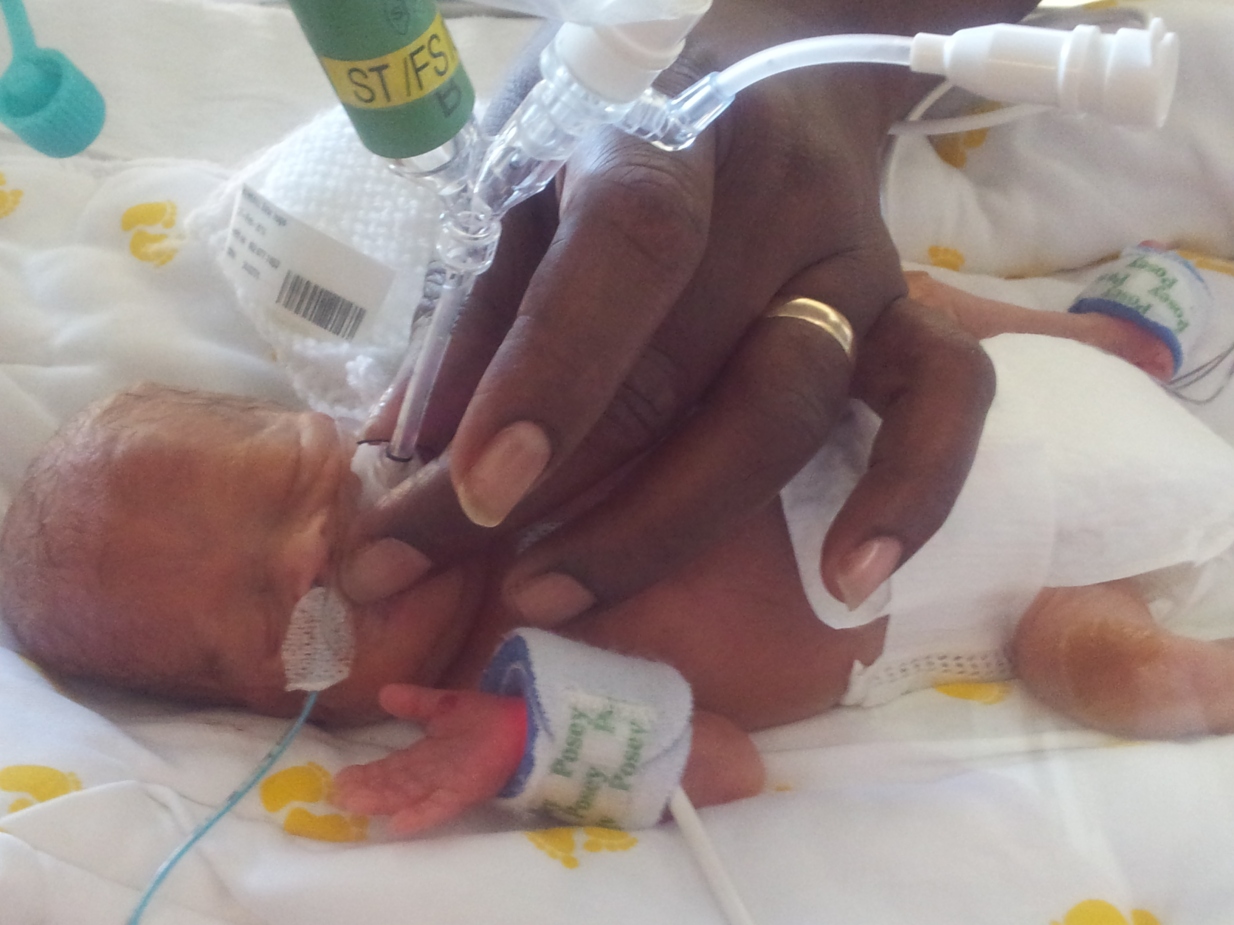
The consultant told me to open the porthole, touch him, get my mummy germs on him. I didn’t want to, I thought I would break him, but I did, I reached in with my hand and my son gripped my finger. It was the most amazing moment ever.
So began the most beautiful and the most terrible 33 and a bit days of my life. Hugo lived for 35 days, but I missed a day and a half of it.
That was Friday February 21 2014. Ten months ago to the day. There are many parts of the story I do not remember, but the terror of that wheelchair journey and the ecstasy of finally meeting my son are two moments that are etched in my memory forever.
I made a formal complaint: the written reply felt flippant to me, that they did not fully understand the gravity of the situation, the potential implication of their inaction. I met with representatives of the ward a couple of months later and read them the riot act. They will never forget me, nor Hugo. No other mother should experience that. Having HELLP syndrome and everything else that went with it was bad enough. That was unavoidable. My life was saved, Hugo given the best chance. I am grateful for every moment I had with Hugo.
But what happened on that ward that day was entirely avoidable.
I have felt a compulsion to write this today. I don’t know why: perhaps I just need to get it out of my head, in a raw, visceral way.
I know I am lucky to be here. The ‘heartburn’ and pain under my ribs was my liver in serious trouble. My kidneys weren’t doing well either. My blood pressure was far too high and my platelet level far too low.
Here I sit, 10 months later. Physically sound, thanks to the actions of the wonderful maternity, obstetric, anaesthetic and pathology teams of two hospitals.
Emotionally, I am still trying to process it. Pregnancy is supposed to be a natural event. I know bad things can happen during pregnancy: babies lost, babies tragically born sleeping. But the placenta turning your body against you? The placenta sending toxins around your body, shutting down your organs. I know now it is not my fault, but it does not prevent me feeling guilty.
HELLP. What a crappy acronym.
There is nothing helpful about it.
It is a difficult thing to get your head around.