There have been some fantastic conversations taking place on the MatExp Facebook group, with lots of ACTION threads being posted to generate discussion. The aim of these discussions is to identify ways that we can ACT to improve maternity experiences. Big, long-term actions that might require system change or a change in culture. And small, immediate actions, that professionals and individuals can take today to improve the maternity experience of those around them.
As a result of the day to day experiences of the mums on my Facebook group, I have been in touch with a number of senior health visitors to discuss the service and how it can potentially be improved. I presented to a group of health visiting managers in Greater Manchester last week, thanks to an invitation from Jill Beswick, and have been asked to speak to the new health visiting students at MMU in the autumn. For some of my thoughts on health visiting please see these three posts on my personal blog:
Health Visiting: Quality and Quantity
Health Visiting: Tell Us About It
Health Visiting: Keeping Everyone Happy?
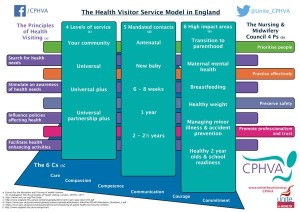
Jenny Harmer has written this very useful blog post about what a health visitor’s role entails. In terms of a family’s maternity experience, it is the health visitor who is responsible for their care for the first five years of the child’s life, and they certainly focus on the 1001 Critical Days, or from conception to age 2. They are currently focused on transition to parenthood, breastfeeding, healthy weight and maternal mental health (as well as accident prevention and school readiness) – these are topics crucial to a family’s maternity experience and issues that crop up again and again when families discuss postnatal care.
So we would hope that health visitors are working closely with midwives and other birth professionals to ensure a smooth transition to parenthood and ongoing care and support. Unfortunately, this is not what parents are routinely reporting, as I mentioned in my blog post for Sheena Byrom’s series, What The National Maternity Review Team Needs To Know. When I introduced this topic on the #MatExp Facebook group I asked:
- Midwives – are you aware of the health visitor’s role, their 6 High Impact Areas and the ways in which they can help families? Are you aware that many now offer antenatal visits? How do you work with health visitors, hand over to them and so on?
- Health Visitors – those who are already doing antenatal visits, are these done in conjunction with communication with the family’s midwifery team? How do you work with midwives postnatally to ensure a smooth handover for families?
- Parents – how well did your midwifery and health visiting teams work together? Have you examples of best practice? Where are the gaps?
- Everyone – how can we ACT to make improvements in this area?
The actions suggested were:
- Pathways to be put in place for communication and handover from midwives to health visitors
- Close working relationships between midwives and HVs so that each team can phone the other to access additional support for families
- Student midwives to go on visits with health visitors to understand why collaborative working is so important
- Best practice is for HV teams to have monthly meetings with midwives and GPs, and for midwives to ring the HV team about every discharge so they have a full picture for postnatal contact
- Joined up IT systems – HVs currently use different systems to the maternity units, so they have no chance to check through maternity notes and only receive basic demographic information about families
- Continued and consistent support for mums re infant feeding during the first six weeks
- 7 day a week health visiting service to truly meet the needs of families
- NNU and other hospital departments to inform health visitors if babies have been born early or sick so that HV can offer support to the family
- Websites with all of the local maternity information for families, including health visiting services; better signposting from all NHS teams to other groups and sources of support available to families
- Midwives to inform mothers at booking and during pregnancy that they will be offered an antenatal visit from the health visitor, and that it’s a good opportunity to discuss pregnancy and feeding methods, alongside other parenting issues. If it was part of the schedule given it would become normal – antenatal appointments with HVs are now offered to all pregnant women and dads/partners are encouraged to be present – it’s a holistic assessment
- Midwife @JennytheM commented “I was on a study day about supporting vulnerable families and the importance of contacting the Health Visitor in such cases was reiterated – an electronic discharge pings to a GP and I’m going to find out if that can also go to the Health Visitor = instant information about discharge – which would help prevent communication failures.”
NHS England (West Midlands) has launched a campaign to raise awareness of the role of health visitors: http://www.bcpft.nhs.uk/about-us/news-and-events/529-campaign-launches-to-raise-awareness-of-health-visitors-and-thier-five-key-visits I hope HV teams continue to clarify their role in this way, both to families and to other birth professionals.
Commissioning of health visiting services moved from NHS England to local authorities on 1st October 2015. It is important that the birth community and families alike recognise what HVs have to offer so that their services continue to be provided across the country. Health visiting teams are responsible for 100% of children born in the UK. It is a massive remit, and one that can have a significant impact on public health if used to its full capacity.
Helen Calvert
@heartmummy
2015